
Across the region’s urban, rural and suburban communities, the top health concern is poverty. It drives health inequities that undermine wellness and cut lives short more than any other single cause of illness, according to an extensive new report by Common Ground Health, the health research and planning organization for the Rochester-Finger Lakes region.

“We’ve failed to understand the extent to which poverty deprives whole populations of vigor and longevity,” said Wade Norwood, CEO of Common Ground Health. “As much as we all talk about poverty, as much as we all talk about health, we’ve kept them completely apart.”
Overloaded: The Heavy Toll of Poverty on Our Region’s Health aims to close that gap. The report connects the dots between life lived on the financial edge and appalling health inequities – unfair and avoidable sickness and death linked to income, race and other factors. It weaves together health data, personal stories and analysis of more than 6,800 responses to Common Ground’s My Health Story survey conducted in 2018.
The research shows that the conditions and stresses of poverty compromise the physical and emotional wellbeing of residents every day, from exposure to mold, lead and other toxins common in substandard housing to the psychological strain of trying to make ends meet. The study found that by nearly every metric, residents of the Finger Lakes with scarce financial resources experience alarmingly worse health outcomes.
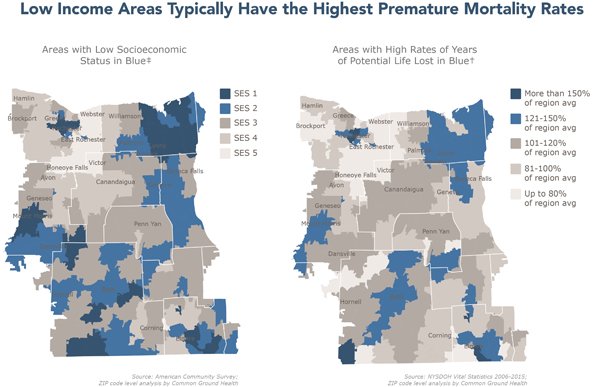
The report’s findings include:
- The estimated cost of health inequity exceeds $1 billion annually for our region.
- More years of life are lost to health inequity than all forms of cancer combined.
- Residents of high poverty neighborhoods die eight years earlier on average than residents of low poverty neighborhoods.
- Compared to residents with household incomes over $75,000, those with incomes under $20,000 are 105% more likely to lose their teeth, 154% more likely to have diabetes, and 224% more likely to be diagnosed with depression.
“Poverty is a public health issue that knows no geographic boundaries,” said Diane Devlin, public health director for Wayne County, noting that roughly equal number of people in poverty are living in our region’s rural, suburban and urban communities. “No matter where they live, cash strapped residents have a hard time affording transportation, safe housing and nutritious foods, which are fundamental to health,” she said.

“Health and wealth are tightly intertwined,” said Leonard Brock, executive director of the Rochester-Monroe Anti-Poverty Initiative. “As much as poverty puts folks at higher risk for diabetes, hypertension, asthma and other chronic illnesses, poor health also compromises a person’s ability to earn a living wage. It’s an unfair cycle that traps individuals,” he said.
The report concludes that investing in interventions to address the root causes of health inequities is imperative. In addition, it notes that the region has a proud history of public health success and an unusually strong tradition of collaboration across the health care ecosystem.
Building on this legacy, and with its new report guiding the discussion, Common Ground calls for collaboration across geographies, sectors, backgrounds and perspectives to challenge the tangle of structural inequities that currently lead to poor health.
View and download the Overloaded report here.
Download data visualizations from the report here.
Related coverage:
Rochester Business Journal New report shines light on poverty outside the city
Minority Reporter Poverty is a real killer
13 WHAM-TV Report finds strong link between health, poverty in Rochester
WROC-TV Study: Health care inequality a burden on Rochester's economy
WXXI News Finger Lakes poverty is driving early deaths, report finds
WHEC-TV Study finds poverty is region's biggest health concern

